Joshua Adeyoju1, Parwez Hossain1,2
1Faculty of Medicine, University of Southampton, Building 85, Life Sciences Building, Highfield Campus, Southampton, SO17 1BJ
2Southampton Eye Unit, University Hospital Southampton NHS Foundation Trust
Abstract
Introduction
The femtolaser has emerged as a novel method to conduct anterior segment surgery in ophthalmology, including deep anterior lamellar keratoplasty (DALK) surgery. There are certain advantages the femtolaser may have, as compared to manual/conventional methods for DALK corneal transplant surgery.
Methods
This literature review aims to identify both observational and interventional studies within femto-DALK literature, and as such, discuss indications, surgical techniques, outcomes and scope for further research in the area. Studies were identified via thorough online database text word searching.
Results
Common indications for femto-DALK match that in conventional-DALK literature. In outcomes, the femtolaser can produce equivalent visual outcomes as seen in conventional-DALK. Some interventional studies show statistically significantly better visual outcomes than conventional-DALK. Complication rates with conventional-DALK appear to be equivalent.
Two surgical techniques, the Anwar and the Melles technique, are popular in femto-DALK. Surgical opinion in literature appears to find the Anwar technique advantageous in femto-DALK. Two graft shapes are popular in femto-DALK, a 90 degree side-cut and a mushroom shaped graft, although there is a lack of direct interventional research comparing the two.
Conclusion
There is a wealth of research within femto-DALK literature which aids the current landscape. There remains scope for further research within femto-DALK including in study design, outcomes measured, and surgical techniques assessed. As femtolaser technology continues to develop, there may be further differences observed within literature as time progresses.
Introduction
The keratoplasty, or corneal transplant, is one of the oldest transplant surgeries in the world. The procedure replaces the patient’s (host) cornea with a healthy donor cornea. Keratoplasties have an important role as one of the only, and the best treatment, for corneal pathologies that severely affect sight. Conventionally, surgeons use a trephine, a specialised handheld blade, to make cuts in both host and donor tissue for keratoplasty.
Corneal pathologies may only affect certain layers of the cornea and so varying depths of corneal transplant have been developed. Lamellar keratoplasties are partial thickness transplants, as opposed to full-thickness penetrating keratoplasties (PK). This review will focus on deep anterior lamellar keratoplasty (DALK), a further subset of lamellar keratoplasty that only transplants anterior corneal tissue. DALK is seen as more technically challenging than a penetrating keratoplasty but is also associated with quicker recovery and lower rejection rates.
The femtosecond laser/femtolaser is an infrared laser capable of ultra-short duration pulse of 10-15 seconds and beam width of just 8 microns (1). Utilised in various ophthalmic procedures, its first documented use in keratoplasty (both penetrating and lamellar) was in 2000 (1), essentially replacing the trephine as a surgical knife for host and donor incisions. The femtolaser’s physical characteristics gives a theoretical advantage over trephination – it penetrates tissue with little collateral damage and can produce various geometric shapes, increasing graft-host surface area and strength (2).
The femtolaser’s potential in keratoplasty explains the ongoing research assessing the laser as an alternative to trephination. One of the main drawbacks to conventional DALK is the extensive learning curve and technical difficulties behind the intricate procedure (3). Femto-DALK could well help standardise such an operation (3), and the femtolaser’s physical properties, described above, could improve patient recovery time and visual outcomes (4).
Aims and Methods
This review shall focus on the literature of femto-DALK studies in principle, with thematic focus to:
- Discuss indications and key
- Outcomes of femto-DALK studies in comparison with trephine
- Discuss surgical techniques and cuts used in femto-DALK research
- Discuss what further research appears to be needed
The reviewed literature is derived from 12 online database searches, including PubMed, Medline and EBSCO. Keywords such as femtosecond, laser, deep anterior lamellar keratoplasty and trephine were used in text word searches.
Why Femto-DALK?
It is important to mention findings from femto-DALK case series to recognize the rationale behind comparative femto-DALK studies. Of several femto-DALK case series analysed, the studies’ individual disseminations were unanimous in the following principles:
- Femto-DALK is a safe surgical alternative to conventional PK and DALK (5,6)
- Femto-DALK is efficacious, producing expected clinical improvement in visual outcomes (5,6)
- The need for prospective, comparative studies comparing conventional trephination to femto-DALK is warranted (5,6)
Indications and outcomes of femto-DALK vs conventional DALK
Comparative studies comparing femto-DALK to conventional DALK were congruent in terms of only including those with keratoconus, either advanced or non-advanced. Observational studies also mainly performed their surgeries on those with keratoconus/other corneal ectatic disorders, with small numbers treating corneal scarring (5,7). This matches literature on the conventional DALK method, which has been accepted to be the gold standard for corneal diseases like keratoconus where the corneal endothelium is still intact and need not be transplanted.
To discuss the studies’ outcomes, results are presented in tables and in text. All studies showed improved visual outcomes in consecutive follow up points for femto-DALK and conventional-DALK.
Studies were consistent in assessing visual acuity and astigmatism and/or keratometry as primary outcomes and so this information is displayed in tables 1-3. All studies statistically compared outcomes at a 95% confidence level – p value > 0.05 was seen as statistically significant. All studies calculated a mean average bar Shehadeh-Mashor et al., who used median.
Table 1: Visual acuity outcomes of studies comparing femto-DALK to conventional-DALK
| Alio et al. | Bleriot et al. | Shehadeh-Mashor et al. | Li et al. | |||||
|---|---|---|---|---|---|---|---|---|
| Femto | Conventional | Femto | Conventional | Femto | Conventional | Femto | Conventional | |
| Visual Acuity 1m | 0.30 | 0.39 | - | - | - | - | - | - |
| Visual Acuity 3-4m | - | - | 0.27 | 0.27 | 0.30 | 1.00 | - | - |
| Visual Acuity 6-8m | 0.45 | 0.52 | 0.26 | 0.17 | 0.30 | 0.31 | 0.23 | 0.30 |
| Visual Acuity 12m | 0.55 | 0.54 | 0.14 | 0.25 | 0.23 | 0.30 | 0.08 | 0.13 |
Table 2: Astigmatism or refraction outcomes of studies comparing femto-DALK to conventional-DALK m = months post-surgery, D = dioptres Bold results indicate a statistically significant difference (p<0.05)
| Alio et al. | Bleriot et al. | Li et al. | ||||
|---|---|---|---|---|---|---|
| Femto | Conventional | Femto | Conventional | Femto | Conventional | |
| Astigmatism/ refraction 1m (D) | 5.16 | 5.30 | 4.00 | 4.25 | - | - |
| Astigmatism/ refraction 6m (D) | 4.60 | 4.79 | 4.00 | 3.00 | - | - |
| Astigmatism/ refraction 12m (D) | 5.43 | 4.62 | 3.75 | 2.50 | 5.35 | 6.63 |
Table 3: Keratometry outcomes of studies comparing femto-DALK to conventional-DALK m = months post-surgery, K = keratometry standard of measure Bold results indicate a statistically significant difference (p<0.05)
| Bleriot et al. | Li et al. | |||
|---|---|---|---|---|
| Femto | Conventional | Femto | Conventional | |
| Keratometry 4m (K) | 46.30 | 47.10 | - | - |
| Keratometry 8m (K) | 45.30 | 46.70 | - | - |
| Keratometry 12m (K) | 45.40 | 46.50 | 43.24 | 48.31 |
Alio et al. followed up both arms (FS-DALKn: 25 eyes, conventional DALKn: 10) of their study at 1 month, 6 months and 1 year (8). They found no statistically significant difference between either arm of their study at any time-point for best corrected distance visual acuity or cylinder refraction topography. This study was unique in qualitatively measuring the healing of host-graft wound interface post-surgery. An independent observer, at an unstated time-point, graded the wound healing as grade 0-4, with 0 being a ‘transparent scar’ and 4 ‘signifying opacity with significant cosmetic imbalance’. The closer a scar is to grade 4 the better in terms of healing activity. This study found healing to be more evident in the FS-group with more eyes at grade 3 and 4 (p < 0.05).
Bleriot et al. followed up both arms (FS-DALKn: 19, conventional DALKn: 17) of their study at 1, 4, 8 and 12 months. No statistically significant difference was found between arms at any time-point in visual acuity nor keratometry. A statistically significant difference was noted in mean suture management duration, defined as the time between removal of first and last corneal wound suture (FS-DALK: 119 days, conventional-DALK: 470) (9).
Li et al. followed up both arms (FS-DALKn: 94, conventional-DALKn: 100) at 6 and 12 months (10). It is noted their cohort is far larger than other studies. The femtolaser did statistically significantly better at 6 and 12 months for best corrected visual acuity, 12 month astigmatism, 12 month keratometry and endothelial healing time (FS-DALK: 3 days, conventional-DALK: 6 days).
Shehadeh-Mashor et al. followed up both arms (19 eyes in each arm) at 3, 6 and 12 months (11). The femtolaser did statistically significantly better in 3 month best corrected visual acuity than the conventional group. All other time-points in visual acuity, spherical equivalent refraction (12 month FS-DALK: -3.0 dioptres, conventional-DALK: 0.0 dioptres) and astigmatism showed no significant difference. Full suture removal occurred at a mean of 9.1 months in the FS-DALKs, which was statistically significantly longer than the conventional-DALK’s 4.9 month figure, and at contrast with Bleriot et al’s results. This study presented their averages as medians.
Complications of femto-DALK vs conventional DALK
Bleriot et al. and Shehadeh-Mashor et al. both experienced a relatively high number of complications, in both arms of their studies. The two studies saw intraoperative macro/micro perforations of posterior corneal tissue. A further myriad of postoperative complications occurred, laid out in table 4. Shehadeh-Mashor et al. noted there was no statistically significant difference in complication rates between their two arms. Li et al. experienced no complications in either group, while Alio et al.’s study did not present complication outcomes.
Table 4: Complications reported in studies comparing femto-DALK to conventional-DALK
| Bleriot et al. | Shehadeh-Mashor et al. | Li et al. | |||||
|---|---|---|---|---|---|---|---|
| Femto | Conventional | Femto | Conventional | Femto | Conventional | ||
| n | 19 | 17 | 19 | 19 | 94 | 100 | |
| Intraoperative Complications | Microperforations | 3 | 1 | - | - | - | - |
| Incomplete big bubble | 4 | - | - | - | - | - | |
| Descemet’s membrane perforations | - | - | 3 | 2 | - | - | |
| Postoperative Complications | Raised intra-ocular pressure | 5 | 5 | 6 | 3 | - | - |
| Exposed sutures | 1 | 9 | - | - | - | - | |
| Glaucoma medication for over 12 months post-op | 2 | 1 | - | - | - | - | |
| Descemet’s membrane detachment | - | - | 2 | 5 | - | - | |
| Rejection | - | - | 3 | 2 | - | - | |
| Delayed epithelial healing | - | - | 1 | 1 | - | - | |
| Central serous retinopathy | - | - | 1 | - | - | - | |
Surgical techniques and cuts of femto-DALK research
There is an apparent heterogeneity observed in the surgical research of femto-DALK, in two methodological aspects – the surgical technique itself and the shape of the graft.
Various surgical techniques have been proposed for the technically challenging DALK, and of these two prove to be popular – the Anwar (or big-bubble) technique (12) and the Melles technique (13). The Anwar technique involves the injection of an air bubble into a corneal side cut to separate the Descemet’s membrane (posterior corneal layers) from the stroma. The Melles technique involves draining the anterior chamber of the eye, replacing it with air, creating a reflection for the surgeon. The surgeon uses the reflection as a guide on how deep to make corneal side cut incisions. In conventional DALK surgery the two techniques are seen as having no statistically significant difference in main postoperative outcomes (14) – but no studies exist that methodically compare the two techniques in femto-DALK. Conventional DALK has been shown to have a steep learning curve for the surgeons (15).
Disparate surgical techniques were used in femto-DALK studies (interventional and observational). Two studies used only Anwar technique on their patients (8,9). Two studies used the Melles technique (7,16). Two studies incorporated hallmarks of Anwar and Melles into bespoke techniques (17,18). Two studies used either Anwar or Melles depending on surgical preference (6,11). One study did not use either technique (10).
Some surgeons believe the femtolaser has an advantage (over trephination) in the Anwar technique as the femtolaser’s uniform and precise recipient graft cuts allow an accurate channel to gauge the depth at which to inject air (3,8,9). In Lu et al.’s (18) observational case series, they propositioned this advantage resulted in their high rate of achieving successful big bubble insertion (no intraoperative perforations). At 90.7% it was above the commonly touted 80-90% success rate seen in conventional big-bubble/Anwar technique DALK (19).
Li et al.’s study was unique in not performing either Anwar or Melles technique as they felt that with their cohort of eyes (with thin corneas) the risk of perforation was too high.
The femtolaser is capable of producing a variety of geometric graft shapes. In femto-DALK literature, two graft shapes predominate – a straight cut, 90 degree side-cut and a ‘mushroom’ shape graft, in which the graft anterior diameter is greater than the posterior diameter. These graft shapes are illustrated in figure 1.
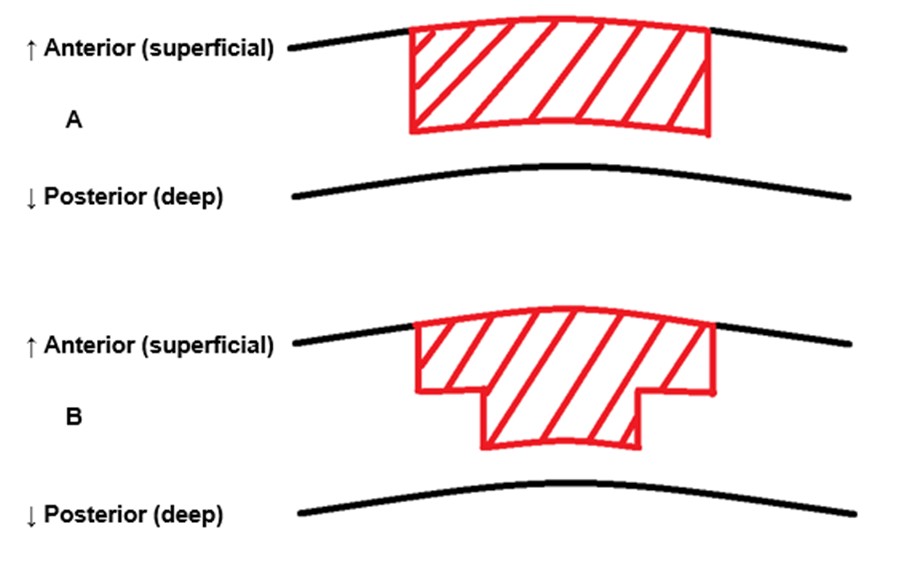
As well as the advantages mentioned in section 1.1 (the 90 degree side cut is used in the conventional method), the mushroom has been theorised to have a further advantage over the 90 degree side-cut as it retains more posterior host tissue (20). This is of importance in DALK, whereby it is already considered a gold standard for anterior corneal diseases. Other surgeons have commented that the mushroom shape is superior over other femto-shapes as there is no ambiguity in the placing of the graft into the dissected host cornea (6), and it allows for easy intra-operative control of posterior tissue perforation (17).
An editorial by ophthalmologist Baradaran-Rafii (21) noted the lack of randomised controlled comparison between the shapes capable in femto-DALK. Indeed, there is a lack of any real comparative literature. Of the comparative (DALK vs conventional) studies observed, Alio et al. and Shehadeh-Mashor et al. both used a mushroom shape, which perhaps gives another dimension to their significant results in corneal wound healing and visual acuity, respectively. The remaining comparative studies used a 90 degree side-cut, although Li et al. still utilised femtolaser properties to make the side-cut oblique, which trephines cannot do.
Scope for further research
The scope for further research is a clear theme that is discussed not only in femto-DALK literature but is also clear to the reviewer of the literature in this manuscript. The nature of corneal transplantation techniques make the procedure, as a whole, intrinsically variable. There are biological, mechanical, immunological, environmental and surgical variables that may impact on a corneal transplant’s success. The femtolaser’s dynamism has, in part, also added to this variability – there are now different shapes capable in corneal transplant surgery and one must also take into account the different femtolasers available on the market, each with different pulse rates, pulse durations, spot sizes and pulse energies.
A logical follow up would see an RCT comparing femto-DALK and conventional-DALK, allowing experimental control in these confounding variables. The literature of femto-DALK suggests this, with references to the need for larger (10), randomised (18) comparative samples, that are prospective (5,7) in nature – the four comparative studies in this review were retrospective in design.
In regards to graft shape and surgical technique, as implied previously, there are further avenues in research. Shehadeh-Mashor et al. discussed that further research is needed to evaluate the mushroom graft shape they used (6). While an RCT exists comparing the Anwar and Melles techniques in conventional-DALK (14), no such study exists in femto-DALK, although surgical opinion appears to favour the Anwar technique in femto-DALK.
Suture techniques often vary between studies, as well as the reporting of suture removal, an important part of the postoperative care of the corneal transplant. This has been noted in femto-DALK literature, with comments that comparative research in suture technique and removal needs further research, especially given one of the theorised advantages of femto-DALK could be sutureless postoperative care (22).
Despite the theory of increased biomechanical stability in the cornea for femto-DALK as compared to conventional-DALK, there is little in vivo femto-DALK studies that measure this. This is commented on in a meta-analysis of corneal biomechanical stability post-DALK (23). Alio et al.’s study measured wound healing activity at the graft-host junction. In some ways this may be seen as assessing corneal biomechanical stability, especially as it is linked with early suture removal. However, the measuring of corneal hysteresis and corneal resistance factor, both known to be a valid gauge corneal biomechanical stability (23), is not seen in femto-DALK in vivo literature.
A number of papers comment on the femtolaser’s high cost (10), and how a medico-economics study evaluating the cost-effectiveness of the machinery is warranted (9). On the other hand, some ophthalmologists speculate the femtolaser could save money and resources when used in lamellar surgery as the same donor cornea could be used for posterior and anterior lamellar surgery.
Although different studies use different femtolasers (each having different properties), this is not stated as an avenue for future research in femto-DALK literature. One imagines this is due to practical (some brands of femtolaser take up a large amount of space and are not portable) and/or financial reasons. However, some studies have discussed scope for improvements in femtosecond-laser properties to facilitate femto-DALK procedures. Bleriot et al. (9) called for improved programmability in future femtosecond lasers, and Li et al. (10) recorded their femtolaser could not perform cuts of different thickness simultaneously in central and peripheral cornea.
Opinion appears to be hopeful that newer systems will be more cheap, precise and practical4. Progression in technology is clear as older papers have seen their suggestions for femtolaser improvement realised, eg. Soong & Malta’s 2009 review hoped for more portable systems4, with certain models having this feature as of 2011 (24). Similarly, W.D. Chamberlain’s editorial from 2011 (25) documented their hope for femtolasers that are able to perform cataract, corneal and refractive surgery on the same machine (with view to the financial benefits of such an apparatus). As of 2018 some models of femtolaser are capable of this (3).
Conclusion
In summary, the femtolaser can produce equivalent visual outcomes as seen in conventional-DALK reproducibly and reliably. In some occasions it performs statistically significantly better than comparative conventional-DALK groups for visual outcomes. Complication rates with conventional-DALK appear to be equivalent.
Two surgical techniques, the Anwar and the Melles technique, are popular in femto-DALK. Surgical opinion in literature appears to find the Anwar technique advantageous in femto-DALK. Two graft shapes are popular in femto-DALK, a 90 degree side-cut and a mushroom shaped graft. Surgical opinion in literature finds the mushroom shape favourable but there is a lack of comparative literature.
There is further scope for research in femto-DALK in regards to prospective, randomised trials comparing femto-DALK to conventional-DALK, the study of different graft shapes, different surgical techniques, corneal biomechanical stability and in medico-economic analysis. There is also hope for further advancements in femtosecond technology itself in the context of keratoplasty surgery.
Acknowledgements
Thank you to Prof Parwez Hossain for his help and support in the writing of this review. This manuscript was an output from first author, JA’s integrated MMedSci degree.
References
1. Roszkowska AM, Urso M, Signorino A, et al. Use of the Femtosecond Lasers in Ophthalmology. 2018;167.
2. Cimberle M. Femtosecond laser technology enhances corneal grafting. Ocular Surgery News US Edition.
3. Mehta JS. Deep Anterior Lamellar Keratoplasty With the Femto LDV Z8. Cataract and Refractive Surgery Today, 2018:1-2.
4. Soong HK, Malta JB. Femtosecond Lasers in Ophthalmology. American Journal of Ophthalmology 2009;147 (2):189-97.e2.
5. Almousa R, Samaras KE, Khan S, et al. Femtosecond laser-assisted lamellar keratoplasty (FSLK) for anterior corneal stromal diseases. Int Ophthalmol 2014;34 (1):49-58.
6. Shehadeh-Mashor R, Chan C, Yeung SN, et al. Long-term outcomes of femtosecond laser-assisted mushroom configuration deep anterior lamellar keratoplasty. Cornea 2013;32 (4):390-95.
7. Chan CCMD, Ritenour RJMDF, Kumar NLBMPH, et al. Femtosecond Laser-Assisted Mushroom Configuration Deep Anterior Lamellar Keratoplasty. Cornea 2010;29 (3):290-95.
8. Alio JL, Abdelghany AA, Barraquer R, et al. Femtosecond Laser Assisted Deep Anterior Lamellar Keratoplasty Outcomes and Healing Patterns Compared to Manual Technique. Biomed Res Int 2015;2015:397891.
9. Bleriot A, Martin E, Lebranchu P, et al. Comparison of 12-month anatomic and functional results between Z6 femtosecond laser-assisted and manual trephination in deep anterior lamellar keratoplasty for advanced keratoconus. J Fr Ophtalmol 2017;40 (6):e193-e200.
10. Li S, Wang T, Bian J, et al. Precisely Controlled Side Cut in Femtosecond Laser-Assisted Deep Lamellar Keratoplasty for Advanced Keratoconus. Cornea 2016;35 (10):1289-94.
11. Shehadeh-Mashor R, Chan CC, Bahar I, et al. Comparison between femtosecond laser mushroom configuration and manual trephine straight-edge configuration deep anterior lamellar keratoplasty. Br J Ophthalmol 2014;98 (1):35-9.
12. Anwar M, Teichmann KD. Big-bubble technique to bare Descemet’s membrane in anterior lamellar keratoplasty. J Cataract Refract Surg 2002;28 (3):398-403.
13. Melles GR, Rietveld FJ, Beekhuis WH, et al. A technique to visualize corneal incision and lamellar dissection depth during surgery. Cornea 1999;18 (1):80-6.
14. Baradaran-Rafii A, Eslani M, Sadoughi M-M, et al. Anwar versus Melles Deep Anterior Lamellar Keratoplasty for Keratoconus: A Prospective Randomized Clinical Trial. Ophthalmology 2013;120 (2):252-59.
15. Sherif A Eissa. Analysis of the learning curve of big bubble-deep anterior lamellar keratoplasty by a single corneal surgeon. Delta Journal of Ophthalmology 2016;17 (3):128-32.
16. Espandar L, Mandell JB, Niknam S. Femtosecond laser-assisted decagonal deep anterior lamellar keratoplasty. Canadian Journal of Ophthalmology 2016;51 (2):67-70.
17. Fung SS, Aiello F, Maurino V. Outcomes of femtosecond laser-assisted mushroom-configuration keratoplasty in advanced keratoconus. Eye (Lond) 2016;30 (4):553-61.
18. Lu Y, Yang L, Xue C, et al. Femtosecond laser-assisted deep anterior lamellar keratoplasty with big-bubble technique for keratoconus. Indian journal of ophthalmology 2016;64 (9):639-42.
19. Feizi S, Javadi MA, Daryabari S-H. Factors influencing big-bubble formation during deep anterior lamellar keratoplasty in keratoconus. British Journal of Ophthalmology 2016;100 (5):622-25.
20. Levinger E, Trivizki O, Levinger S, et al. Outcome of “mushroom” pattern femtosecond laser-assisted keratoplasty versus conventional penetrating keratoplasty in patients with keratoconus. Cornea 2014;33 (5):481-5.
21. Baradaran-Rafii A, Hasani H. Different techniques for performing DALK: are they making a real difference? British Journal of Ophthalmology 2014;98 (10):1311-12.
22. Baradaran-Rafii A, Eslani M. Femtosecond laser-assisted corneal transplantation. British Journal of Ophthalmology 2013;97 (6):675-76.
23. Jiang M-SP, Zhu J-YMD, Li XMD, et al. Corneal Biomechanical Properties After Penetrating Keratoplasty or Deep Anterior Lamellar Keratoplasty Using the Ocular Response Analyzer: A Meta-Analysis. Cornea 2017;36 (3):310-16.
24. Reggiani-Mello G, Krueger RR. Comparison of commercially available femtosecond lasers in refractive surgery. Expert Review of Ophthalmology 2011;6 (1):55-65.
25. Winston D. Chamberlain. How FLAK is changing keratoplasty. Review of Ophthalmology, 2011.
